| Valve and Conduit Replacements |
|
|
 |
|
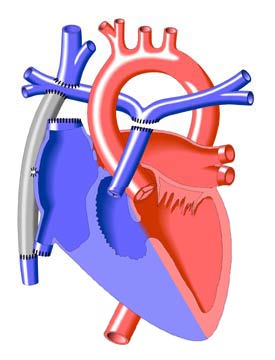
The Fontan Operation - Extracardiac
The Fontan Procedure is the third and final procedure for separating the left and right-sided circulations in single ventricle lesions. It allows the passive flow of venous blood directly into the pulmonary arteries (total cavo-pulmonary connection).
In this procedure, a pathway (or tunnel), usually made of Gore-Tex®, is inserted to connect the inferior vena cava to the pulmonary artery. This tunnel may be constructed either inside (lateral tunnel) or outside (extracardiac Fontan (see illustration)) of the right atrium.
Conduit Repair and Replacement after the Fontan
It is important that the Fontan patient be monitored for proper function of the implanted conduit. Conduits may develop obstructions because of kinking, thrombus (blood clots), or the formation of fibrous tissue in growth (scarring). When an obstruction is suspected, a catheterization may be performed to determine the degree and location of the narrowing.
The obstruction may often be relieved by the insertion of a stent during a cardiac catheterization procedure. However, most surgically implanted conduits will require replacement 10-20 years after insertion.
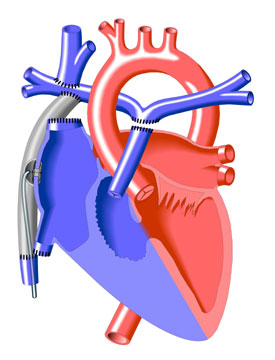
Transcatheter Closure of Fontan Fenestration
At the time of initial Fontan surgery, a small opening (fenestration) may be left in the extracardiac connecting tunnel. This connects the tube and the right atrium to allow excess blood flow to enter the heart if pressure in the pulmonary arteries is too high immediately after surgery. When no longer required, the hole can be closed in the cardiac catheterization laboratory without the need for surgery (see illustration at right). (Approximately 25% of Fontan fenestrations will close spontaneously.)
Small septal occluders, such as the 4-5mm Amplatzer® or 17mm Cardioseal® devices are used to close Fontan fenestrations. The devices are introduced during cardiac catheterization after careful angiographic and echocardiographic determination of the fenestration location. |
|
 |
|