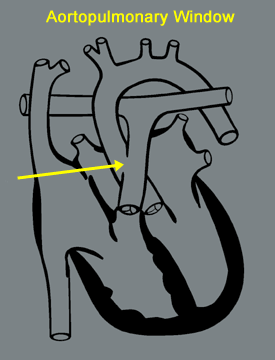
 (rollover to compare with normal)
(rollover to compare with normal) |
|
What Are Its Effects?
The movement of blood from the aorta into the pulmonary artery results in excessive blood flow to the lungs, causing high pulmonary blood pressure. The larger the hole, the greater the volume of blood shunted and the more severe the symptoms.
The symptoms that are associated with this defect depend on the size of the window. Small windows often cause enlargement (dilatation) of the left ventricle and/or heart failure and are characterized by a continuous heart murmur. The more common large aortopulmonary windows result in cyanosis (blueness caused by oxygen poor arterial blood) affecting the whole body, pulmonary hypertension, and Eisenmenger Complex.
If not diagnosed soon enough, some children can develop sustained high pulmonary blood pressure (pulmonary hypertension) secondary to changes in growth of the pulmonary arteries. This severe result of an Aortopulmonary Window can render some children inoperable.
An aortopulmonary window may be overlooked in childhood, especially if pulmonary hypertension is present, and because it often occurs with other more common defects, such as PDA, ventricular septal defect (VSD), atrial septal defect (ASD), Tetralogy of Fallot, or aortic stenosis. Most windows are large, so that, if not recognized in early childhood, they will cause a significant left to right shunt, often resulting in pulmonary hypertension. Therefore, they are frequently associated with high pulmonary blood pressures and pulmonary vascular obstructive disease (PVOD) when first diagnosed in the adult patient.
Echocardiography is used to make the diagnosis and to determine the amount of left to right shunting. A cardiac catheterization procedure may be used to measure the degree of pulmonary hypertension and resistance, if present. |