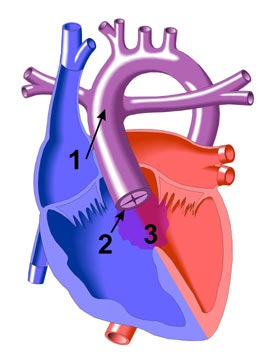
1. Truncus Arteriosus (Type 3)
2. Abnormal Truncal Valve (4 leaflets)
3. Ventricular Septal Defect (VSD) |
|
Truncus Arteriosus and the Adult Patient
This defect almost always requires treatment in early life. Early symptoms are usually severe and include sweating, rapid breathing, inability to feed, arrhythmias (abnormal heart beats), mild cyanosis (blueness), and congestive heart failure. In the absence of treatment, these symptoms, or others that may develop somewhat later, such as pulmonary vascular disease, will almost always prove fatal in early childhood.
In the past, the excessive pulmonary blood flow characteristic of Truncus Arteriosus (also known as Common Arterial Trunk) was reduced by the insertion of a pulmonary band on one or both of the pulmonary artery branches. However, the prognosis was not good after this procedure and it has now been replaced in most cases by open-heart surgery. This involves the separation of the pulmonary and systemic circulations, either by the insertion of conduits and/or patches or by the attachment of part of the pulmonary artery to the right ventricular outflow tract.
In the years after surgery, stenosis (narrowing) or deterioration of the conduits or patches that were used in surgical repair may occur. Replacement of the conduit often becomes necessary, sometimes more than once before a patient reaches adulthood. In some cases, the stenosis can be treated by the insertion of a stent during a cardiac catheterization procedure. Patients with an adequate sized conduit commonly experience deterioration of the valve with combined pulmonary stenosis and insufficiency and may require the insertion of a pulmonary valve either surgically or by a transcatheter approach (Melody® valve).
Another later complication with this defect is dysfunction (regurgitation) of the aortic (truncal) valve, even after repair. A valve replacement operation may eventually be needed. Also, the effects of surgery and irregularities in the ventricular outflow tracts sometimes cause ventricular dysfunction. This may result in arrhythmias, though these conduction anomalies are not characteristic of Truncus Arteriosus. Sometimes, heart block occurs, requiring the insertion of a pacemaker.
The ventricular septal defect (VSD) that is present with this defect is normally patched early in life. Sometimes, a residual VSD persists, requiring surgical closure.
The Truncus Arteriosus patient should be monitored regularly to guard against the development of complications or new symptoms. Testing will generally include an electrocardiogram (ECG), chest x-ray (to check for possible enlargement of the heart), and echocardiogram (to assess various aspects of cardiac function). Exercise testing, echo Doppler testing, MRI (Magnetic Resonance Imaging), use of a Holter monitor, and/or other examinations may also be utilized.
In some cases, a cardiac catheterization procedure may be performed. This will allow the determination of the internal heart anatomy and hemodynamic situation (blood pressures and concentration of oxygen and other gases within the heart).
Despite the variety of late complications after surgery for this defect, the long-term prognosis is good and improving. A recent study of patients who received repair operations before the age of one showed that more than 80% were still alive 20 years after surgery, with all of the deaths occurring during the first 12 years. |